Tobacco kills more than 7 million people each year, including an estimated 1.6 million non-smokers exposed to second-hand smoke.1 It is estimated that tobacco costs the global economy more than $1.4 trillion a year in healthcare costs and lost productivity.2 This World No Tobacco Day, we are going to explore the appeal behind smoking tobacco and the healthcare burden it causes.
What is World No Tobacco Day?3
World No Tobacco Day is a global awareness event, held every year on the 31st May by the World Health Organisation (WHO). The event was created to draw global attention to the tobacco epidemic and the preventable deaths and diseases it causes. Each year follows a new theme; the theme for 2026 is Unmasking the appeal – countering nicotine addiction. Whilst global tobacco use has declined in recent years, its burden remains devastating.
The appeal: Why tobacco still attracts users.

Whilst evidence does not support this, smoking is still widely perceived as a stress reliever, with studies indicating that between 36-43% of people believe smoking helps manage stress, anxiety and depression. The truth is, smoking actually increases tension and lowers mental health in the long run.4
Marketing tactics have changed over the years with the introduction of vapes, flavoured products, and targeting youth and young adults, especially in low-income communities and regions with weaker tobacco regulations.
Together, these psychological misconceptions and evolving marketing strategies create a powerful and carefully engineered appeal. Nicotine products are framed as tools for coping, symbols of independence, or fashionable accessories, rather than addictive substances. These influences normalise use, particularly among younger and more vulnerable populations, making tobacco appear not only acceptable but desirable.
The health burden: What tobacco really costs.
Smoking tobacco has a direct impact on health and is linked to diseases like:5
- Lung cancer,
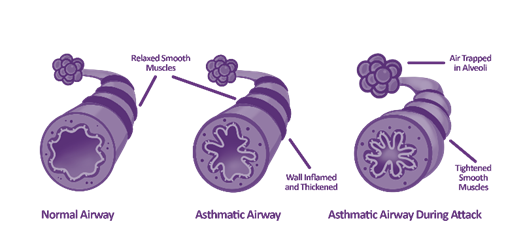
- Chronic obstructive pulmonary disease (COPD),
- Coronary artery disease,
- Stroke.
This doesn’t just impact the smokers themselves; non-smokers are also affected by second-hand smoke, leading to a significant impact on healthcare systems worldwide.
Smoking-related hospital admissions and care in the UK alone cost the NHS £1.9 billion each year, signifying an urgent need for change.6
What needs to change?
There are many contributing factors that could change and improve outcomes worldwide, and whilst there are already various initiatives in place, such as:
- Plain packaging,
- Smoke-free zones,
- Less advertisement.
More can be done across the board to remove the appeal.
Awareness campaigns like World No Tobacco Day help to raise awareness of the significant impact smoking can have on health and economic costs. Additionally, smoking cessation programmes can provide support for those looking to quit smoking. These services can educate smokers on the long-term benefits of quitting smoking as well as highlight tools which can aid a quit attempt. One of those tools is carbon monoxide (CO) monitoring.
What is CO monitoring?

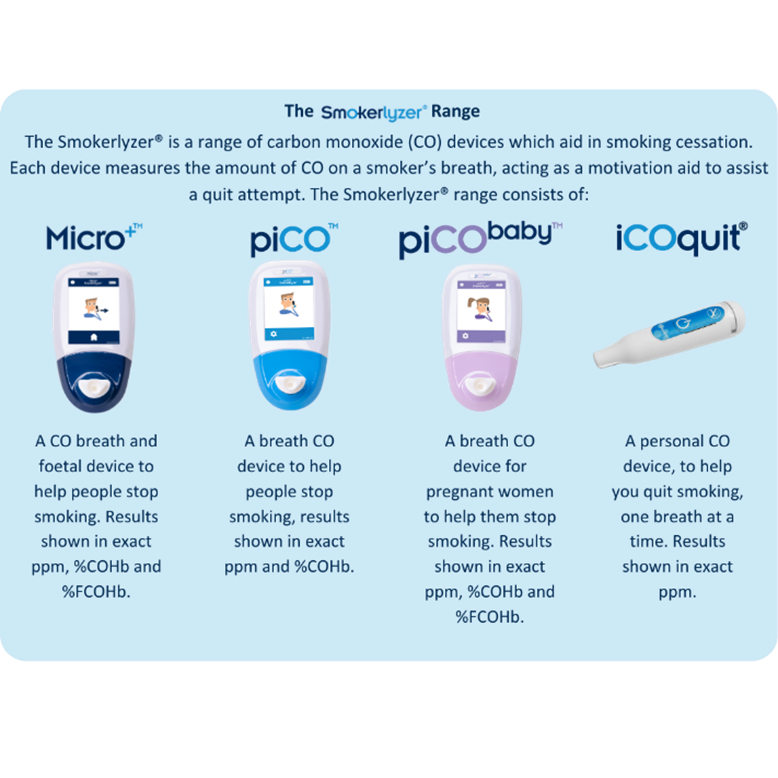
When someone smokes tobacco, they inhale CO, which enters their bloodstream and reduces oxygen delivery around the body.7 A CO monitoring device like the Smokerlyzer® measures CO levels in a person’s exhaled breath. The Smokerlyzer® is widely used across the world as a motivational tool to aid a quit-smoking attempt. Seeing CO levels drop empowers smokers to continue their quit-smoking journey.

A 2012 study found that people who used a CO monitoring device reported feeling more motivated to quit smoking. Participants described how seeing their CO levels decrease over time provided clear, tangible evidence that their efforts were making a real difference. This immediate, visible feedback appeared to strengthen their commitment to quitting by reinforcing the health benefits of staying smoke-free and encouraging them to keep going, especially during moments of doubt or temptation.8
World No Tobacco Day 2026 is highlighting how the appeal to nicotine and tobacco addiction is engineered and not accidental. With healthcare and economic costs rising, it is vital that more is done to tackle the tobacco epidemic.
To learn more about the support available to aid a quit smoking attempt, visit the NHS website here.
To find out more about the Smokerlyzer® range and how it is helping people quit smoking for good, visit the website here.
References
- World Health Organization. Tobacco [Internet]. World Health Organization. World Health Organization; 2025. Available from: https://www.who.int/news-room/fact-sheets/detail/tobacco
- US$ 1.4 trillion lost every year to tobacco use – New tobacco tax manual shows ways to save lives, money and build back better after COVID-19 [Internet]. www.who.int. Available from: https://www.who.int/news/item/12-04-2021-1.4-trillion-lost-every-year-to-tobacco-use-new-tobacco-tax-manual-shows-ways-to-save-money-and-build-back-better-after-covid-19
- World. World No Tobacco Day 2026: Unmasking the appeal – countering nicotine and tobacco addiction [Internet]. Who.int. World Health Organization: WHO; 2025. Available from: https://www.who.int/news/item/17-10-2025-world-no-tobacco-day-2026–unmasking-the-appeal—countering-nicotine-and-tobacco-addiction
- Perski O, Theodoraki M, Cox S, Kock L, Shahab L, Brown J. Associations between smoking to relieve stress, motivation to stop and quit attempts across the social spectrum: A population survey in England. Kaye JT, editor. PLOS ONE [Internet]. 2022 May 17;17(5):e0268447. Available from: https://journals.plos.org/plosone/article?id=10.1371/journal.pone.0268447
- ASH. Smoking and Other Health Conditions – ASH [Internet]. ASH. 2025. Available from: https://ash.org.uk/resources/view/smoking-and-other-health-conditions
- Action on Smoking and Health. Latest figures show cost of smoking in England up 25% to at least £21.8 billion [Internet]. ASH. 2024. Available from: https://ash.org.uk/media-centre/news/press-releases/latest-figures-show-cost-of-smoking-in-england-up-25-to-at-least-21-8-billion
- Raub JA, Benignus VA. Carbon monoxide and the nervous system. Neuroscience and Biobehavioral Reviews [Internet]. 2002 Dec 1;26(8):925–40. Available from: https://pubmed.ncbi.nlm.nih.gov/12667497/
- Beard E, West R. Pilot study of the use of personal carbon monoxide monitoring to achieve radical smoking reduction. Journal of Smoking Cessation. 2012 Jun;7(1):12-7.